Inspired by Ter et al 2026.[1] Photo by How-Soon Ngu on Unsplash. CIPN – chemotherapy-induced peripheral neuropathyEA – electroacupunctureMSKCC – Memorial Sloan Kettering Cancer CenterCTCAE – common terminology criteria for adverse events (from the US NCI)NCI – National Cancer Institute (US)ADLs – activities of daily livingMA – manual acupunctureNPSI – neuropathic pain symptom inventoryVAS – … Continue reading Acupuncture for CIPN 2026
Category: Clinical practice
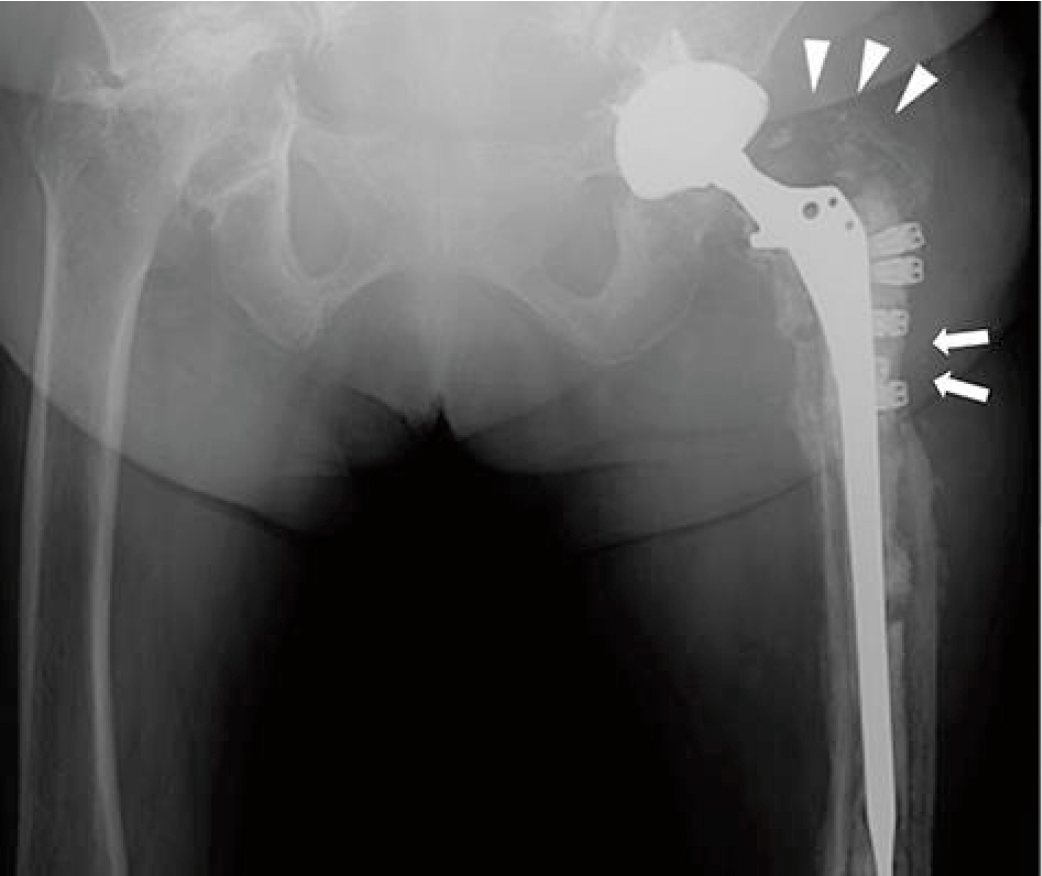
Acupuncture and arthroplasty 2026
Stimulated by Yuasa et al 2026.[1] Figure 3a from Yuasa et al 2026.[1] AE – adverse eventTHA – total hip arthroplastyTKA – total knee arthroplastyIF – impact factorIV – intravenousCLAP – continuous local antibiotic perfusionCRP – C reactive proteinGT – greater trochanterRCT – randomised controlled trial – key to acronyms This is the first AE … Continue reading Acupuncture and arthroplasty 2026
TEAS vs metoclopramide for PONV 2026
Stimulated by Zheng et al 2026.[1] This is one of the colour versions of the Fashion variety. I think a black one like this was used in the trial. TEAS – transcutaneous electrical acupuncture point stimulationPONV – post-operative nausea and vomitingIF – impact factorRCT – randomised controlled trialIV – intravenousGA – general anaesthesiaNRS – numerical … Continue reading TEAS vs metoclopramide for PONV 2026
Acupuncture plus donepezil in AD 2026
Stimulated by Kong et al 2026.[1] An elderly man gazes thoughtfully at Shanghai's skyline during sunset – an AI generated image. AD – Alzheimer’s diseaseRCT – randomised controlled trialIF – impact factorCDR – clinical dementia ratingMA – manual acupunctureEA – electroacupunctureADAS-cog 12 – AD assessment scale, cognitive subscale, 12 item versionMMSE – mini mental state … Continue reading Acupuncture plus donepezil in AD 2026
Acupuncture for DOR 2026
Stimulated by Wang et al 2026.[1] AI generated image used in a previous blog post – see SCs in endometriosis pain 2024. DOR – diminished ovarian reserveRCT – randomised controlled trialIF – impact factorCACMS – China Academy of Chinese Medical SciencesAMH – anti-Müllerian hormoneAFC – antral follicle countSAS – self-rating anxiety scaleIQR – interquartile range … Continue reading Acupuncture for DOR 2026
Acupuncture HT and stroke recurrence 2026
Stimulated by Liu et al 2026.[1] Tianjin Eye on the Hai river. Photo by Vishnu Panday on Pexels.com HT – hypertensionRCT – randomised controlled trialIF – impact factorBP – blood pressureSBP – systolic BPDBP – diastolic BPXNKQ – Xing Nao Kai Qiao (needling method and formula for stroke)HXSF – Huo Xue San Feng (needling method and … Continue reading Acupuncture HT and stroke recurrence 2026
EA for SF-NR 2026
Stimulated by Wei et al 2026.[1] Image from Slashme on Wikipedia.This is an image of the fruit of Myristica fragrans (nutmeg) split open to show the seed with the surrounding aril (also known as mace). I cannot help thinking it looks a bit like a heart. EA – electroacupunctureSF-NR – slow flow / no-reflow (refers to inadequate myocardial perfusion post-PCI)PCI … Continue reading EA for SF-NR 2026
Acupuncture and endocarditis 2026
Stimulated by Zhang and Yi 2026.[1] Photo by Omer Salom on Unsplash. SAE – serious adverse eventIF – impact factorSBE – subacute bacterial endocarditisIE – infective endocarditisPID – prolapsed intervertebral discIV – intravenousMRSA – methicillin-resistant Staphylococus aureusMSSA – methicillin-sensitive Staphylococus aureus – key to acronyms This is a SAE report from Beijing, China, published in the American Journal … Continue reading Acupuncture and endocarditis 2026
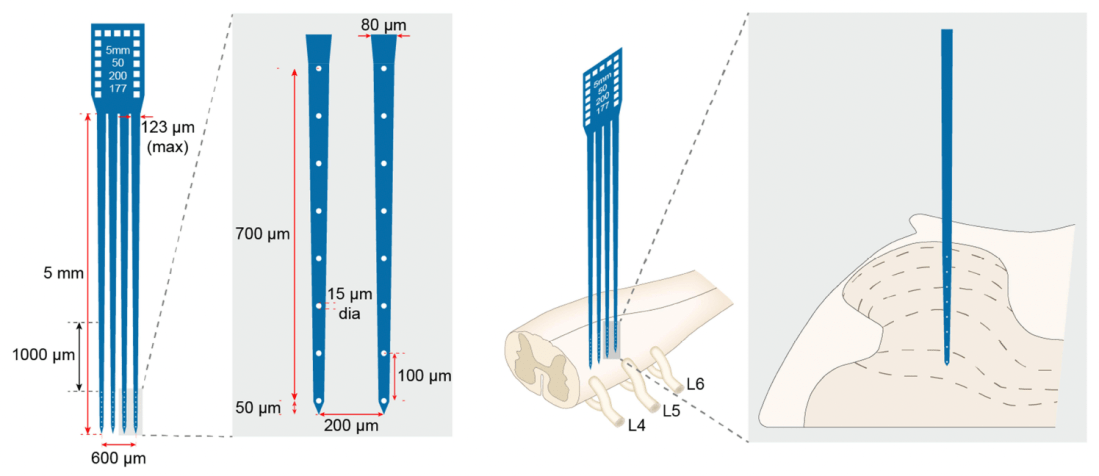
Contralateral EA and descending controls 2026
Stimulated by Zhang et al 2026.[1] Figure 1 from Yu et al 2023.[2] EA – electroacupunctureIF – impact factorWDR – wide dynamic rangeSD – Sprague DawleyCFA – complete Freund’s adjuvant (an oily antigenic mixture including heat-killed mycobacteria)PWR – paw withdrawal thresholdAAV – adeno-associated virusRVM – rostral ventromedial medullaGABA – gamma amino butyric acidChR2 – channel rhodopsin … Continue reading Contralateral EA and descending controls 2026
Acupuncture and insomnia in lung cancer 2026
Stimulated by Yu et al 2026.[1] Photo by Matthew Zheng on Pexels.com IF – impact factorPSM – propensity score matchingaHR – adjusted hazard ratioECOG PS score – Eastern Cooperative Oncology Group performance status score – key to acronyms This week we are staying with the theme of cancer care but moving from gastric cancer to … Continue reading Acupuncture and insomnia in lung cancer 2026







You must be logged in to post a comment.