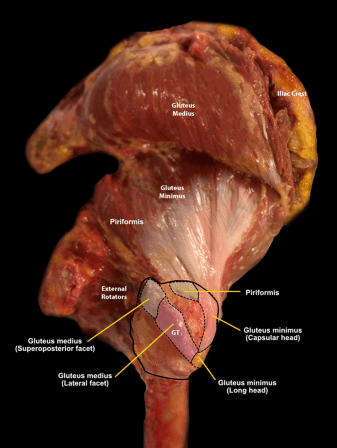
Stimulated by Pinheiro et al and Yi et al 2026.[1,2] Image retrieved by ChatGPT 5.2, but of unknown origin. MSK – musculoskeletalIF – impact factorMRI – magnetic resonance imaging – key to acronyms This week I have chosen a couple of recent anatomical papers that examine innervation patterns in the two lower limb muscles named … Continue reading Gluteus medius and soleus – innervation patterns 2026
Category: Dry needling
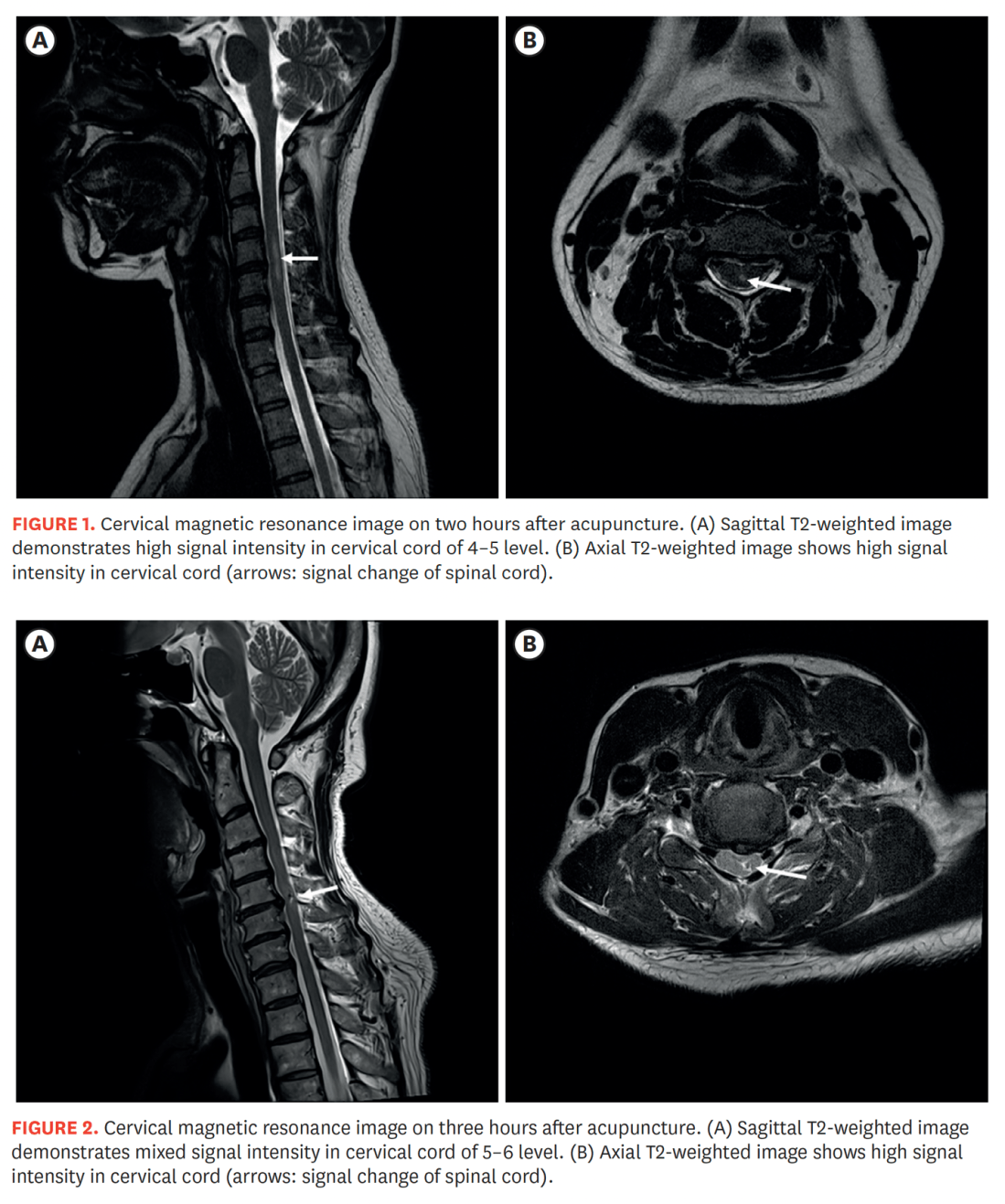
Needling necks and SCI 2025
Stimulated by Kim et al 2025.[1] SCI – spinal cord injury – key to acronym This paper was published in late August this year in the Korean Journal of Neurotrauma, but it has only just come up on my PubMed searches in the last week or so. It is not really extensive enough to devote … Continue reading Needling necks and SCI 2025
EDN in OAK 2025
Stimulated by Dunning et al 2025.[1] Figure 1 from the paper... or you wouldn't have believed me. EDN – electrical dry needlingOAK – OA kneeOA – osteoarthritisIF – impact factorPEDN – periosteal electrical dry needlingPIEDN – periosteal and intra-articular electrical dry needlingEA – electroacupunctureWMA – Western medical acupunctureTENS – transcutaneous electrical nerve stimulationSAE – serious … Continue reading EDN in OAK 2025
Post-acupuncture ACSEH
Stimulated by Wang et al 2025.[1] Photo by Gildo Cancelli on Pexels.com ACSEH – acute cervical spinal epidural haematomapaACSEH – post-acupuncture ACSEHSEH – spinal epidural haematomaIF – impact factorrTPA – recombinant tissue plasminogen activator – key to acronyms I thought this was going to be another first for the blog – a paACSEH mimicking a … Continue reading Post-acupuncture ACSEH
MPS 2025
Stimulated by Steen et al 2025.[1] MPS – myofascial pain syndrome(s)PM&R – physical medicine and rehabilitationMSK – musculoskeletalLS – lumbosacralIF – impact factorTPI – trigger point injectionLA – local anaestheticDN – dry needlingSR – systematic reviewRCT – randomised controlled trialLTR – local twitch responseIMS – intramuscular stimulation – key to acronyms Review papers on MPS … Continue reading MPS 2025
Acupuncture AEs 2024
Inspired by a variety of recent case reports. AI generated image. AEs – adverse eventsPDP – personal development planCXR – chest x ray filmSPs – spinous processesBP – blood pressuremmHg – millimetres of mercury (units of fluid pressure)HR – heart ratebpm – beats per minuteTHA – total hip arthroplastyIBD – inflammatory bowel diseaseESI – epidural … Continue reading Acupuncture AEs 2024
WMA and athletes 2024
Stimulated by Chaabna et al 2024.[1] Photo by Chiara Caldarola on Pexels.com WMA – Western medical acupunctureSR – systematic reviewSM – sports medicineTCA – traditional Chinese acupunctureTCM – traditional Chinese medicine key to acronyms I spent the last weekend teaching on a WMA course in a sports clinic in Porto (HP Clinics), so this paper, … Continue reading WMA and athletes 2024
MSAT for MSK pain
Stimulated by a trip to Jaseng, Seoul, for their 4th annual academic conference, and a paper from the founder of Jaseng, published in Pain 10 years ago, Shin et al 2013.[1] MSAT – motion style acupuncture treatmentMSK – musculoskeletalcLBP – chronic low back painUS – ultrasoundTP – transverse processCAT – conventional acupuncture treatmentRCT – randomised … Continue reading MSAT for MSK pain
Where to needle 2023
…in infraspinatus and other muscles. Stimulated by Lee et al 2023.[1] Possible TrP locations in the infraspinatus muscle based on the frequency of finding EPZs. Yellow indicates the presence of EPZs in 90% to 100% of individuals. Green indicates the presence of EPZs in 50% to 80% of individuals. This is based on data from … Continue reading Where to needle 2023
MTrP needling in GP 2023
Inspired by Yehoshua et al 2023.[1] Needling upper trapezius or GB21 with a subject sitting up and an angle that is tangential to the upper ribcage (from BMAS Points Resource). MTrP – myofascial trigger pointTrP – trigger pointDN – dry needling (mostly MTrP or TrP needling)GP – general practice or general practitioner (whichever is contextually … Continue reading MTrP needling in GP 2023





You must be logged in to post a comment.