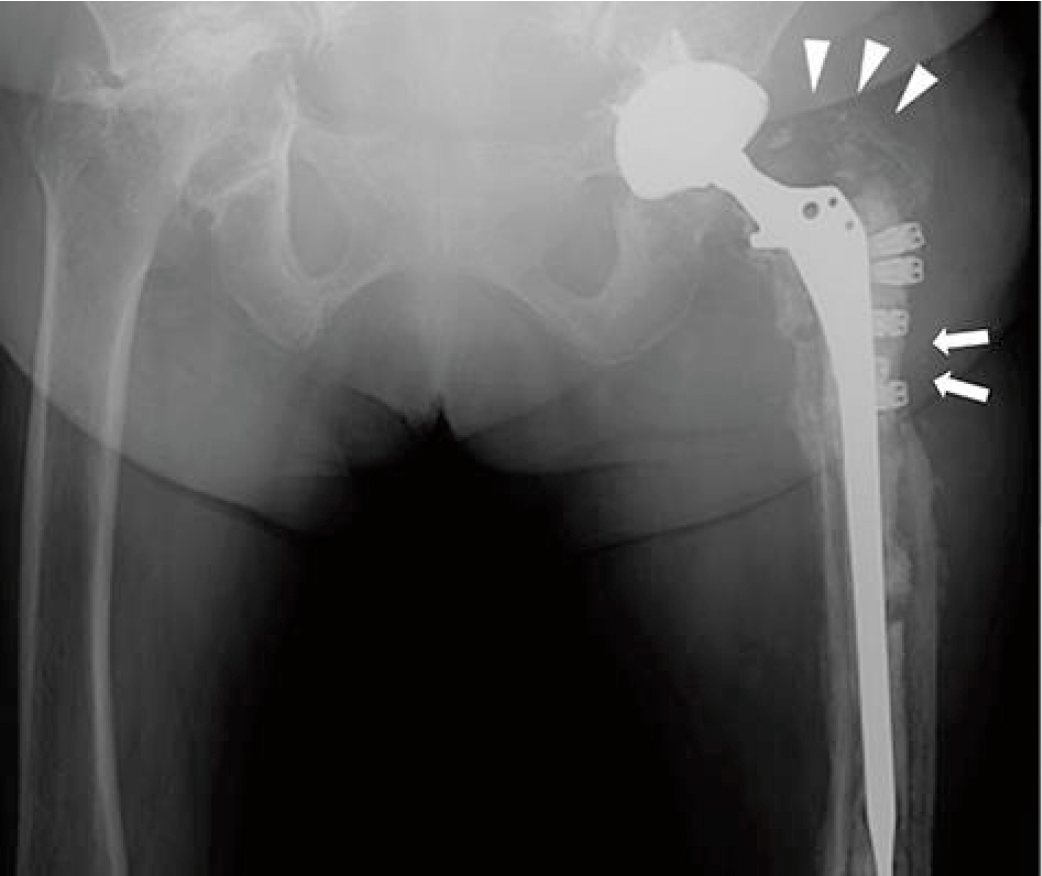
Stimulated by Yuasa et al 2026.[1] Figure 3a from Yuasa et al 2026.[1] AE – adverse eventTHA – total hip arthroplastyTKA – total knee arthroplastyIF – impact factorIV – intravenousCLAP – continuous local antibiotic perfusionCRP – C reactive proteinGT – greater trochanterRCT – randomised controlled trial – key to acronyms This is the first AE … Continue reading Acupuncture and arthroplasty 2026
Category: Adverse events
Acupuncture and endocarditis 2026
Stimulated by Zhang and Yi 2026.[1] Photo by Omer Salom on Unsplash. SAE – serious adverse eventIF – impact factorSBE – subacute bacterial endocarditisIE – infective endocarditisPID – prolapsed intervertebral discIV – intravenousMRSA – methicillin-resistant Staphylococus aureusMSSA – methicillin-sensitive Staphylococus aureus – key to acronyms This is a SAE report from Beijing, China, published in the American Journal … Continue reading Acupuncture and endocarditis 2026
Septic arthritis during chemotherapy
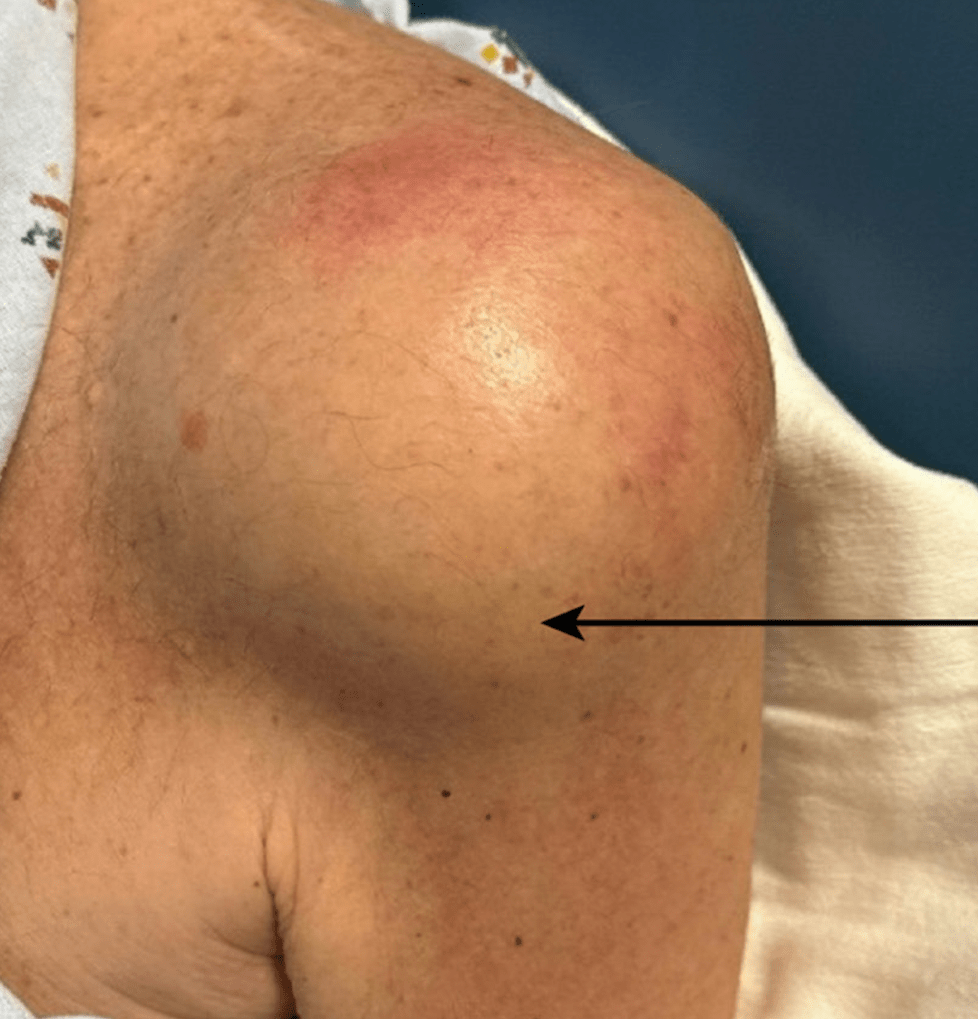
Stimulated by Lester et al 2026.[1] From Figure 1 of Lester et al 2026.[1] IF – impact factorCD – cluster of differentiation (classification for surface antigens on white blood cells) – key to acronyms I have been waiting a long time for an adverse event report of infection following acupuncture in a patient undergoing chemotherapy. … Continue reading Septic arthritis during chemotherapy
Fatal bilateral pneumothoraces 2026
Inspired by Chai et al 2026.[1] Photo by Robina on Unsplash. IF – impact factorBCE – before common eraED – emergency department – key to acronyms This case report comes from Wuhan, China, and reads a bit like an investigative crime novel in places. It was published in the journal Forensic Science, Medicine, and Pathology (IF 1.4), which … Continue reading Fatal bilateral pneumothoraces 2026
Punctured lungs and eyeballs 2025
Stimulated by Reindorf et al and Song et al 2025.[1,2] Figure 1 from Reindorf et al 2025.[1] The red arrow is indicating a small right apical pneumothorax. According to the text of the case report, you are also supposed to be able to see the needle fragment, but they have not given us an arrow … Continue reading Punctured lungs and eyeballs 2025
Needling necks and SCI 2025
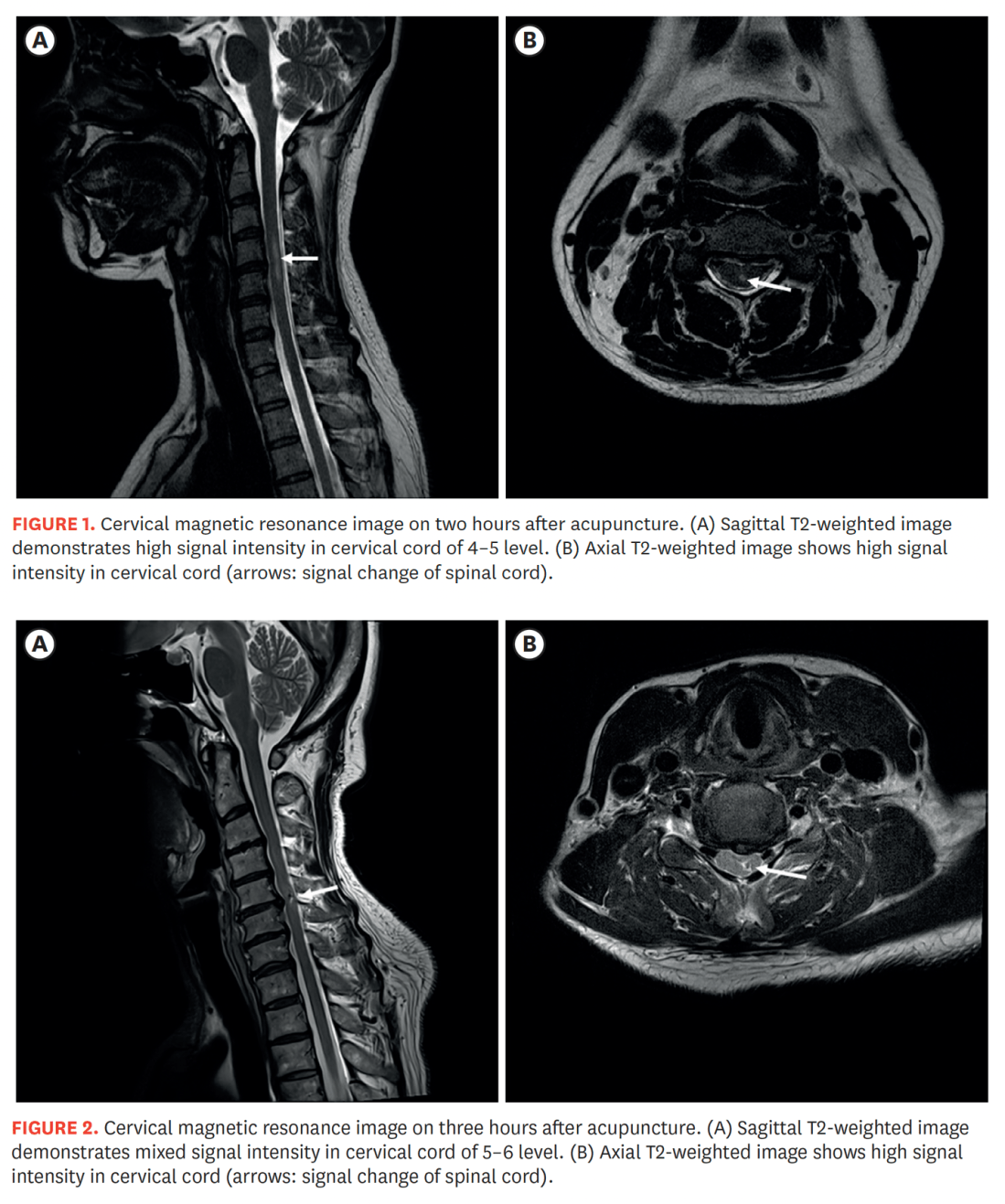
Stimulated by Kim et al 2025.[1] SCI – spinal cord injury – key to acronym This paper was published in late August this year in the Korean Journal of Neurotrauma, but it has only just come up on my PubMed searches in the last week or so. It is not really extensive enough to devote … Continue reading Needling necks and SCI 2025
EDN in OAK 2025
Stimulated by Dunning et al 2025.[1] Figure 1 from the paper... or you wouldn't have believed me. EDN – electrical dry needlingOAK – OA kneeOA – osteoarthritisIF – impact factorPEDN – periosteal electrical dry needlingPIEDN – periosteal and intra-articular electrical dry needlingEA – electroacupunctureWMA – Western medical acupunctureTENS – transcutaneous electrical nerve stimulationSAE – serious … Continue reading EDN in OAK 2025
Post-acupuncture ACSEH
Stimulated by Wang et al 2025.[1] Photo by Gildo Cancelli on Pexels.com ACSEH – acute cervical spinal epidural haematomapaACSEH – post-acupuncture ACSEHSEH – spinal epidural haematomaIF – impact factorrTPA – recombinant tissue plasminogen activator – key to acronyms I thought this was going to be another first for the blog – a paACSEH mimicking a … Continue reading Post-acupuncture ACSEH
Periocular and ocular AEs 2025
Inspired by Davidson et al, Tsai et al, and Yao et al 2025.[1–3] Photo by Cameron Venti on Unsplash. AEs – adverse eventsBCVA – best corrected visual acuityRCT – randomised controlled trial – key to acronyms AEs related to needling close to the eyes occur from time to time, and I have mentioned them here a couple of … Continue reading Periocular and ocular AEs 2025
Acupuncture AEs 2024
Inspired by a variety of recent case reports. AI generated image. AEs – adverse eventsPDP – personal development planCXR – chest x ray filmSPs – spinous processesBP – blood pressuremmHg – millimetres of mercury (units of fluid pressure)HR – heart ratebpm – beats per minuteTHA – total hip arthroplastyIBD – inflammatory bowel diseaseESI – epidural … Continue reading Acupuncture AEs 2024






You must be logged in to post a comment.