Inspired by Wen et al 2021.[1]

EA – electroacupuncture
ket to acronyms
MA – manual acupuncture
IR – insulin resistance
PCOS – polycystic ovary syndrome
RCT – randomised controlled trial
BMI – body mass index
HOMA-IR – homeostatic model assessment of insulin resistance
FPG – fasting plasma glucose
FINS – fasting insulin
TA – true acupuncture
DD – double dummy
IQR – interquartile range (25th to 75th value, the median being the 50th value out of 100)
CIs – confidence intervals (95% of subjects are within the 95% CIs of the mean)
MoA – mechanism of action
AUC – area under curve
SHA – self home acupuncture
This was a moderately large (n=342) sham controlled comparative RCT with 3 parallel arms including a double dummy design. It is a trial that was anticipated in a previous blog: Metabolic effects 2020.
Women were included between the ages of 18 and 40 with BMI ≥18.5 and with PCOS and IR and were randomised to 3 equal sized groups (n=114 per group).
IR was determined by a HOMA-IR value of ≥2.14. HOMA-IR is calculated from fasting plasma glucose (FPG) and fasting insulin (FINS).
HOMA-IR = FPG x FINS / 22.5
True acupuncture (TA) plus placebo metformin was compared with metformin plus sham acupuncture and sham acupuncture plus placebo metformin (the latter being the ‘double dummy’).
The acupuncture treatment was quite intensive with 3 sessions per week for 4 months – 48 sessions in total. The acupuncture involved a mixture of low frequency EA to 8 points in the leg and abdomen (2 midline and 3 bilateral) and MA to a further 6 points (all bilateral). Two similar protocols, each using a total of 14 needles, were alternated. The treatment is described in detail in the published trial protocol.[2]
The sham acupuncture involved 2 points on each upper arm, one on the acromion and the other near the deltoid insertion. The needles used were short and fine and place superficially with no manual stimulation. EA leads were attached, and the device turned on but with the intensity set at zero.
Metformin was given for 4 months in a dose of 500mg three times a day. The dose could be reduced to twice or once a day according to the severity of side effects.
At the end of the 4 months of treatment, the median HOMA-IR had changed very little in the TA and DD groups (it had reduced by 0.1), but it had reduced by 0.8 in the metformin group. However, the median values at baseline differed by 0.6 with IQRs spanning from 2.1 to 3.5. We are presented with medians and 95% CIs for the 4-month data rather than IQRs, and the 95% CIs span 1.1 for all groups, so much narrower…
We are told that the change difference reaches significance for metformin over TA, but the 4-month HOMA-IR is virtually the same for all groups. It looks rather like there was a relevant baseline difference between groups and what might be referred to as a failure of randomisation.
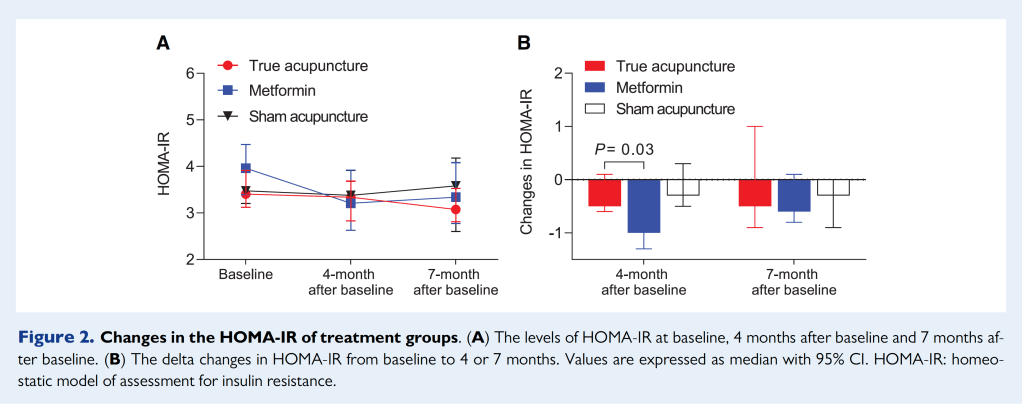
It is interesting that the 7-month data diverges from that at 4 months. The DD group deteriorate by 0.2, the TA group improve by 0.2, and the metformin group deteriorates by 0.1. I may be guilty of over interpreting these trends, but they may indicate a lack of long-term effect for both sham and the drug as opposed to that for true acupuncture.
There were a host of secondary outcomes, and some had highly significant results in statistical terms. BMI reduced more in the metformin group; however, this may be confounded by the fact that over 30% of this group had diarrhoea, over 13% had nausea, 14 suffered vomiting and 11% had a loss of appetite.
The reduction in FINS was significantly larger for the metformin group, but there was a baseline difference and of course this may be related to the MoA of the drug – we don’t know exactly how it works I’m afraid.
…glycaemic control seems better with EA than metformin
TA did best in the FPG levels, with AUC measures being highly significantly lower than the other groups. This is encouraging since it implies that glycaemic control, and thus the risk of developing type 2 diabetes is better with EA than metformin.
Finally, whilst this was an impressive and ambitious piece of research, it seems likely that it was underpowered, since the changes in the TA group did not match those predicted from early results in the pilot project.[3] The number of sessions and the length of the treatment course were both reduced: 72 to 48 sessions and 6 months to 4 months.
It was estimated that there would be a drop of 25% in the HOMA-IR index after 4 months of acupuncture based on a drop of 14% (0.6) after 3 months. That in itself seems ambitious, but in reality, the drop was only 0.34 after 6 months (difference in median values).
The drop in FPGAUC was twice as big in the present study after 4 months of treatment than in the pilot study after 6 months of treatment, so go figure! But at least the baseline values were all very similar across the groups.
The authors suggest the next step might be to combine acupuncture with metformin, presumably to see if it is better than metformin alone. I was thinking about how you could control for all the time and attention from having acupuncture 3 times a week. I came up with a gym membership plan as part of the trial. Everyone goes to the gym 3 times a week, and one group gets 2 hours in the gym plus metformin and the other group gets 1 hour in the gym and a session of EA in the clinic next-door.
Treatment 3 times a week in a clinic or hospital is probably never going to be feasible outside of the Far East, so I would like to try SHA for managing these metabolic issues that need intensive treatment. Before you ask, I would of course plump for my favourite combination of ST36–Zongping pairs bilaterally.
References
1 Wen Q, Hu M, Lai M, et al. Effect of acupuncture and metformin on insulin sensitivity in women with polycystic ovary syndrome and insulin resistance: a three-armed randomized controlled trial. Hum Reprod Published Online First: 15 December 2021. doi:10.1093/humrep/deab272
2 Li J, Ng EHY, Stener-Victorin E, et al. Acupuncture treatment for insulin sensitivity of women with polycystic ovary syndrome and insulin resistance: a study protocol for a randomized controlled trial. Trials 2017;18:115. doi:10.1186/s13063-017-1854-2
3 Li J, Wu W, Stener-Victorin E, et al. A prospective pilot study of the effect of acupuncture on insulin sensitivity in women with polycystic ovary syndrome and insulin resistance. Acupunct Med 2020;38:310–8. doi:10.1177/0964528420902144
You must be logged in to post a comment.